Article checked, partially written, and source verified by Journalist Rosalba Mancuso.
For many years, scientists have been searching for a neuroprotective therapy that could stop the progression of Parkinson’s disease. But while we have many treatments that manage symptoms—like tremors or stiffness—we don’t yet have a way to stop the brain’s cells from declining.
However, a new study called NADPARK, published in Cell Metabolism, has ignited a new wave of hope. Led by researchers at the University of Bergen, Norway, this randomized Phase I trial investigated whether a specialized form of Vitamin B3—Nicotinamide Riboside (NR)—could penetrate the human brain and reboot the failing energy systems of patients with Parkinson’s.
Nicotinamide Riboside (NR): What Is It?
What it is known as nicotinamide riboside (NR) is, in reality, a new form of Vitamin B3 containing a molecule of ribose sugar. This compound is used to increase the cellular levels of NAD (Nicotinamide Adenine Dinucleotide) in the human body. NAD is, in turn, a coenzyme involved in cell metabolism to produce energy. NAD also contributes to repairing DNA and mitigating damage from oxidative stress and aging.
The common form of vitamin B3 is, instead, known as nicotinamide only. The latter is a water-soluble molecule that dissolves in water.
The main feature of nicotinamide is to boost energy in the brain from the foods we ingest. Vitamin B3 is, in fact, found in eggs, fish, cereals, and meat. Most of the time, this precious vitamin is lost through cooking, depriving the brain of a valuable ally to prevent neurodegenerative diseases like Parkinson’s and Alzheimer’s.
One of the hallmarks of these diseases is the decline in the levels of the aforementioned NAD, now called the anti-aging coenzyme. For your information, coenzymes are molecules derived from vitamins.
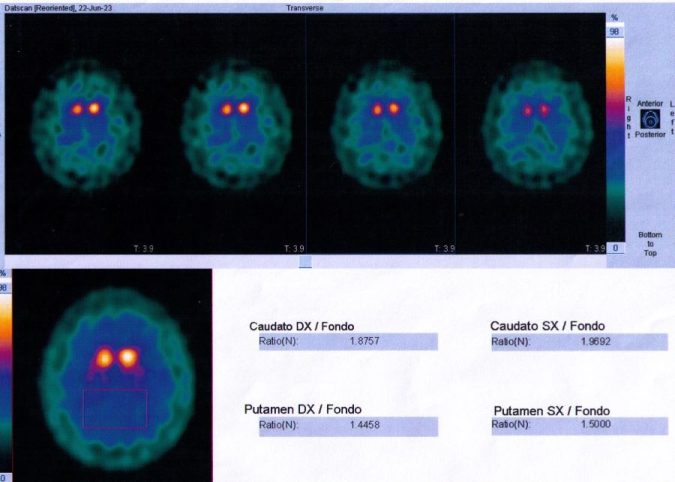
“I also tried vitamin B1 and B3 supplements to ease the side effects induced by my Parkinson’s, and I must admit that when I take them, I feel better. However, the form of Vitamin B3 I use is the water-soluble molecule contained in an effervescent tablet. Of course, if a more advanced molecule of vitamin B3 could stop the progression of Parkinson’s, I would be extremely happy. But the new study is at the beginning, and the results showed to be different from patient to patient,” Journalist Rosalba Mancuso said. She was indeed diagnosed with Parkinson’s in 2023 (see the image of her Brain Scan).
Why NAD Matters
To understand the study, you just need to understand the molecule called NAD (Nicotinamide Adenine Dinucleotide). Every cell in your body relies on NAD to function. As said, it is a coenzyme involved in redox reactions—essentially acting as a shuttle that moves electrons to the mitochondria (power plants of the cell) so they can produce energy (ATP).
In Parkinson’s, these “power plants” begin to fail. This is known as mitochondrial dysfunction. As we age, and particularly in neurodegenerative diseases, NAD levels decline. When NAD levels drop, the cell can no longer repair its DNA, it cannot manage oxidative stress, and it cannot clear out “cellular trash” (misfolded proteins like alpha-synuclein).
The question of the NADPARK team was simple but bold: If we give patients an oral supplement of Nicotinamide Riboside (a precursor to NAD), can we “refill the tank” in the brain and stop the cells from dying?
Why Scientists Preferred Nicotinamide Ribosine Instead of Nicotinamide?
Nicotinamide riboside (NR) is able to penetrate cells better than common nicotinamide. The latter is indeed used as a supplement for skin health, while NR is preferred as a neuroprotective treatment with major efficacy in boosting energy levels and NAD.
Inside the NADPARK Trial: The Methodology
The NADPARK study was a double-blind, randomized, placebo-controlled Phase I trial. While Phase I trials are usually designed just to check for safety, this team went much further.
They enrolled 30 newly diagnosed patients with Parkinson’s who had not yet started traditional dopaminergic medication. This was crucial, as it allowed researchers to see the effect of NR without the “noise” of other drugs. Half the group received 1,000 mg of NR daily for 30 days, while the other half received a placebo.
The researchers used a sophisticated array of “biomarkers” and clinical tests to track the drug’s effect:
- 31P-MRS (Phosphorus Magnetic Resonance Spectroscopy): A specialized MRI that can actually measure the concentration of NAD inside the living human brain.
- FDG-PET Scans: To measure how the brain’s metabolism (glucose use) changed.
- Lumbar Punctures: To see if the NAD metabolites were appearing in the cerebrospinal fluid.
- Muscle and Blood Biopsies: To see how the rest of the body’s “engines” were responding.
The Findings: A Brain Transformed
Fortunately, the study met its primary goal: Oral NR increases NAD levels in the human brain. This is a massive victory because the “blood-brain barrier” often blocks supplements from reaching their target.
1. The Metabolic Shift
One of the most fascinating findings of the study came from the PET scans. In patients whose brain NAD levels increased (whom the researchers called “MRS responders”), there was a significant change in brain metabolism. Specifically, they saw a decrease in glucose uptake in the basal ganglia.
While “decreased glucose” might sound like a bad thing, the researchers interpreted this as a sign of increased efficiency. By boosting NAD, the neurons may have been able to switch to more efficient energy sources (like fatty acid oxidation) or simply perform their duties with less “energy” waste and less sugar consumption.
2. Cleaning the Cellular House
The transcriptomic analysis (looking at gene expression) showed that NR was “turning on” essential survival pathways. Specifically, it induced genes related to:
- The Proteasome and Lysosome: These are the cell’s waste-management systems. In Parkinson’s, these systems usually fail, leading to protein clumps. NR seemed to “rev up” the cleaners.
- Mitochondrial Complex Assembly: The building blocks of the cell’s power plants were being reinforced.
3. Dampening the Fire of Inflammation
Neuroinflammation is a major driver of Parkinson’s progression. The study found that NR recipients had lower levels of inflammatory cytokines in both their blood and their cerebrospinal fluid. By lowering the “heat” in the brain, NR may be creating a more hospitable environment for surviving neurons.
The Clinical Question: Did Patients Feel Better?
Because this was only a 30-day study, the researchers didn’t expect to see a “miracle cure” in terms of physical symptoms. However, they were surprised to find a mild clinical improvement in the MDS-UPDRS scores (the gold standard for measuring Parkinson’s symptoms) among those who had the highest increase in brain NAD.
While it’s too early to say NR is a symptomatic treatment, the correlation between increased brain NAD and better movement is a signal that cannot be ignored.
Not a “One-Size-Fits-All” Response
It is important to note that the response to NR was variable. About 10 out of the 13 NR recipients showed a significant brain NAD increase, while others did not, despite taking the same dose.
This suggests that some people may “absorb” or “utilize” the supplement differently. This variability is a key area for future research. It tells us that in the future, Parkinson’s treatment might be “personalized”.
Looking Ahead: The NOPARK Trial
The NADPARK study was a “Proof of Concept.” It proved that NR is safe, it gets into the brain, and it changes the biology of the disease. But can it truly slow down the disease over the years?
To answer that, the same team has launched a much larger Phase II trial of the NOPARK study, involving over 400 patients followed for a longer period. This trial will be the definitive test to see if NR can become the world’s first true disease-modifying therapy for Parkinson’s.
What This Means for Patients Today
While the medical community generally advises waiting for Phase III results before starting a new supplement regimen, the NADPARK study is a major morale booster for the Parkinson’s community.
It moves the conversation away from simply “replacing dopamine” and toward “protecting the brain.” It highlights the importance of cellular health, mitochondrial support, and the potential of nutritional precursors to act as powerful medicine.
Conclusion
The NADPARK study isn’t just about a Vitamin B3 pill; it’s about a shift in how we view neurodegeneration. By treating Parkinson’s as a “cellular energy crisis,” we open up new avenues for treatment that were previously dismissed.
As we await the results of the NOPARK trial, one thing is clear: the science of NAD has moved out of the petri dish and into the human brain, and the future of Parkinson’s care looks brighter because of it.
Featured image: Courtesy of Rosalba Mancuso
Source:
Brakedal, Brage et al.
Cell Metabolism, Volume 34, Issue 3, 396 – 407.e6
Disclaimer: This article is for informational purposes and does not constitute medical advice. Always consult with a neurologist before adding supplements to a Parkinson’s treatment plan.